Unrelated vs. Sibling Donor Outcomes
Due to several clinical advances, such as more precise HLA typing and advances in patient care, unrelated donor transplant outcomes are now comparable to related donor transplant outcomes in many patient populations. [1,2,3,4,5]
The continued improvement in outcomes has led to an increase in the number of unrelated donor transplants. In 2022, Be The Match® facilitated 6,714 transplants.
Advances
Figure 2 shows landmark one-year survival for a rolling cohort of patients consisting of the specified three-year periods. [6] The data show that one-year transplant outcomes for U.S. patients (all diseases, ages and graft types) with unrelated donors have improved 10 percentage points between transplant periods ending in 2005 and in 2010.
Figure 2. One-Year Survival, NMDP/Be The Match Transplants
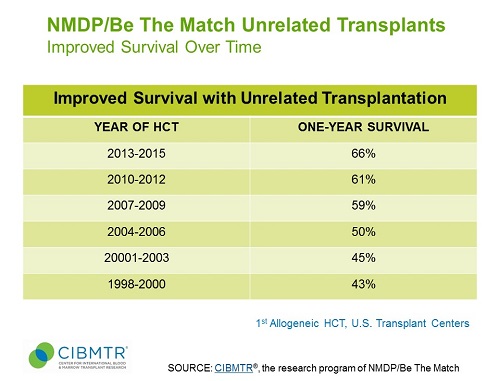
Download Slide: Improved One-Year Survival, Unrelated Donor Transplants
Advances in treating post-transplant complications and more precise HLA matching have contributed to the improvements in survival. [7,8,9] Unrelated donor transplant outcomes are now comparable to related donor transplant outcomes in several patient populations. [1,2,3,4,5]
Due to the increased size and ethnic diversity of the Be The Match Registry® and other donor registries, most patients lacking a suitably matched related donor will be able to find an alternative donor and proceed to transplant.
References
- Mielcarek M, Storer BE, Sandmaier BM, et al. Comparable outcomes after nonmyeloablative hematopoietic cell transplantation with unrelated and related donors. Biol Blood Marrow Transplant. 2007; 13(12): 1499-1507. Access
- Ho VT, Kim HT, Aldridge J, et al. Use of matched unrelated donors compared with matched related donors is associated with lower relapse and superior progression-free survival after reduced-intensity conditioning hematopoietic stem cell transplantation. Biol Blood Marrow Transplant. 2011; 17(8): 1196-1204. Access
- Saber W, Opie S, Rizzo JD, et al. Outcomes after matched unrelated donor versus identical sibling hematopoietic cell transplantation in adults with acute myelogenous leukemia. Blood. 2012; 119(17): 3908-3916. Access
- Robin M, Porcher R, Adès L, et al. Matched unrelated or matched sibling donors result in comparable outcomes after non-myeloablative HSCT in patients with AML or MDS. Bone Marrow Transplant. 2013; 48(10): 1296-1301. Access
- Zhang MJ, Davies SM, Camitta BM, et al. Comparison of outcomes after HLA-matched sibling and unrelated donor transplantation for children with high-risk acute lymphoblastic leukemia. Biol Blood Marrow Transplant. 2012; 18(8): 1204-1210. Access
- CIBMTR Analysis of NMDP Facilitated Transplants 2013. Unadjusted one-year survival of unrelated transplant recipients after first allogeneic transplantation at U.S. transplant centers.
- Lee SJ, Klein J, Haagenson M, et al. High-resolution donor-recipient HLA matching contributes to the success of unrelated donor marrow transplantation. Blood. 2007; 110(13): 4576-4583. Access
- Spellman S, Setterholm M, Maiers M, et al. Advances in the selection of HLA-compatible donors: refinements in HLA typing and matching over the first 20 years of the National Marrow Donor Program Registry. Biol Blood Marrow Transplant. 2008; 14(9, Suppl. 3): 37-44. Access
- Petersdorf EW, Gooley T, Malkki M, Horowitz M. Clinical significance of donor-recipient HLA matching on survival after myeloablative hematopoietic cell transplantation from unrelated donors. Tissue Antigens. 2007; 69(Suppl. 1): 25-30. Access