This study reviewed data from the CIBMTR® (Center for International Blood and Marrow Transplant Research®) registry to examine if using mismatched donors has expanded the availability of hematopoietic cell transplantation (HCT) for ethnically diverse patients. The study reveals that the use of HLA-mismatched donors, particularly haploidentical (haplo) donors, for allogeneic HCT has significantly increased in recent years, enabling more ethnically diverse patients to receive transplantation.
Survival rates have improved across all racial and ethnic groups with the continued innovation in allogeneic HCT field, including increased use of innovative graft-versus-host disease (GVHD) prophylaxis strategies, such as post-transplantation cyclophosphamide (PTCy), and improved supportive care. Despite these advances, the study acknowledges that disease relapse remains a significant concern, highlighting the need for continued research to improve HCT outcomes.
Download a PDF of the study highlights and citation here.
Background
There’s a substantial gap in access to HLA matched donors in allogeneic HCT, particularly among ethnically diverse patients. This study addresses the increasing challenge of finding suitable donors for allogeneic HCT by exploring alternative donor types like cord blood, haplo, and mismatched unrelated donors (MMUD).
These alternatives require overcoming the HLA barrier to prevent GVHD and graft failure. The study used CIBMTR registry data to review HCT activity trends, donor types, and patient outcomes. The primary aim of the study was to determine if the use of alternative donors and novel GVHD prophylaxis regimens, particularly PTCy, has increased access to allogeneic HCT for ethnically diverse patients and to compare the outcomes among these patients with those of non-Hispanic white (NHW) patients.
Study Details
The study analysis included allogeneic HCT recipients in the United States reported to the CIBMTR between 2010 and 2020. In 2020, 8,326 allogeneic HCT procedures were reported, slightly lower than the previous year. Over the last decade, the relative proportions of patients by race and ethnicity receiving allogeneic HCT have remained fairly constant, with an increase in the number of ethnically diverse patients. In 2010, 75% of recipients were NHW, while 13% were Hispanic, and 8% were non-Hispanic Black or African American. In 2020, these proportions changed to 69% NHW, 15% Hispanic, and 9% non-Hispanic Black or African American patients.
Results
This study discovered that the number of transplants decreased by 5% in 2020 compared to 2019, with a decrease in the proportion of NHW patients and an increase in the absolute number of ethnically diverse patients. The use of haplo donors has risen significantly, from 6% in 2013 to 24% in 2020, while cord blood transplants have decreased.
More ethnically diverse groups underwent allogeneic HCT using matched related donors (MRD) compared to matched unrelated donors (MUD). Haplo and MMUD were used in the highest proportion by diverse recipients (see Figure below).
Furthermore, there was a shift towards using PTCy as GVHD prophylaxis, particularly in the haplo and MMUD groups. The study found survival rates for allogeneic HCT patients were highest in the most recent transplantation era (2016-2019) across all racial and ethnic groups.
However, disease relapse remained the most common cause of death post-transplantation for adults and children across all patient groups receiving allogeneic HCT for malignant disease. GVHD was reported more frequently as a cause of death following MUD and MMUD transplants, particularly among Black/African American patients following MUD HCT.
Key Takeaways
This study described several trends in allogeneic HCT, including that the number of allogeneic HCTs decreased in 2020, likely due to the COVID-19 pandemic and its subsequent impacts on health care systems. The use of alternative donor platforms and PTCy for GVHD prophylaxis has increased, enabling more ethnically diverse patients to receive transplants.
Despite the increase in transplantation among ethnically diverse patients, racial and ethnic disparities persist in access to treatment, calling for a holistic approach that addresses social determinants of health and access barriers and promotes patient support services.
The National Marrow Donor Program®/Be The Match® has partnered with the American Society for Transplantation and Cellular Therapy to form the ACCESS Initiative to address and reduce barriers to HCT, ensuring access and outcomes equity for all patients. Though survival rates have improved over recent years for all racial and ethnic groups, more research is needed to understand and improve outcomes post-transplant, especially in the HLA-mismatched setting.
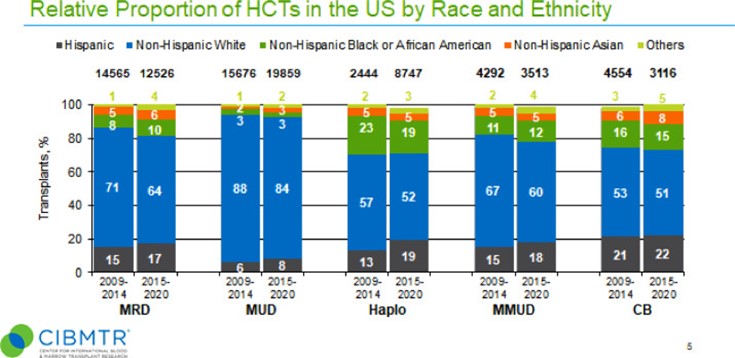
Auletta J, et al., Published in Transplantation and Cellular Therapy
