The Blood and Marrow Transplant Clinical Trials Network (BMT CTN) 1102 study among patients 50–75 years old with intermediate or high-risk myelodysplastic syndromes (MDS), revealed a clear benefit of allogeneic hematopoietic cell transplant (alloHCT) over supportive care. This follow-up study took a closer look at the financial burdens associated with these treatments, particularly evaluating the out-of-pocket (OOP) costs and financial hardships faced by patients undergoing transplant. Researchers found that OOP costs of alloHCT can be substantially higher than in those not receiving HCT and lead to indicators of financial hardship, highlighting the importance of financial support programs to mitigate these concerns.
Background
Transplantation is a costly medical procedure, and financial hardship can often limit access to care or add stress during the recovery process. The BMT CTN 1102 study initially confirmed the advantage of transplantation for older MDS patients but left unanswered questions about the financial implications for patients choosing between transplant and supportive care. A parallel economic evaluation was conducted to shed light on these financial impacts, with participating patients completing a detailed cost diary survey at various stages post-enrollment to capture OOP expenses and financial hardships.
Methods
Out of 216 invited BMT CTN 1102 participants, 138 (64%) consented to the financial study, completing at least one survey. Participants reported their OOP expenses and financial hardships at 1, 7, and 19 months after enrollment. The survey covered costs related to outpatient services, prescription medications, and health care accommodations, along with questions about resorting to savings, borrowing, or incurring debt for health care
Results
Respondents were predominantly male (64%), white (93%), and non-Hispanic (91%), with a median age of 67.7 years. The analysis revealed that, although transplant patients consistently faced higher OOP costs across all categories compared to those receiving supportive care, significant differences were observed only at the 1- and 7-month marks. Total OOP costs were markedly higher for transplant recipients at these times. Moreover, transplant patients experienced greater financial hardship, particularly at 7 months, where a significant portion reported facing at least one hardship indicator.
Key Takeaways
The study's findings highlight a significant financial burden on patients undergoing transplantation for the treatment of intermediate to high-risk MDS. Transplant recipients consistently faced higher OOP expenses compared to those receiving best supportive care, with the greatest disparities observed in the initial months following the transplant. Furthermore, the incidence of financial hardship was notably higher among transplant patients, especially within the first seven months post-treatment. Despite these insights, the limitations posed by the study's relatively small sample size call for further research in larger patient cohorts to validate these findings.
This study underscores the urgent need for the development and implementation of financial navigation and assistance programs. Such initiatives could play a crucial role in alleviating the financial challenges faced by MDS patients considering transplantation, ultimately improving their access to and experience with this potentially life-saving treatment.
Figure
This figure displays OOP costs and financial hardship indicators for transplant and non-transplant (supportive care) patients, with p-values displayed for significant relationships only.
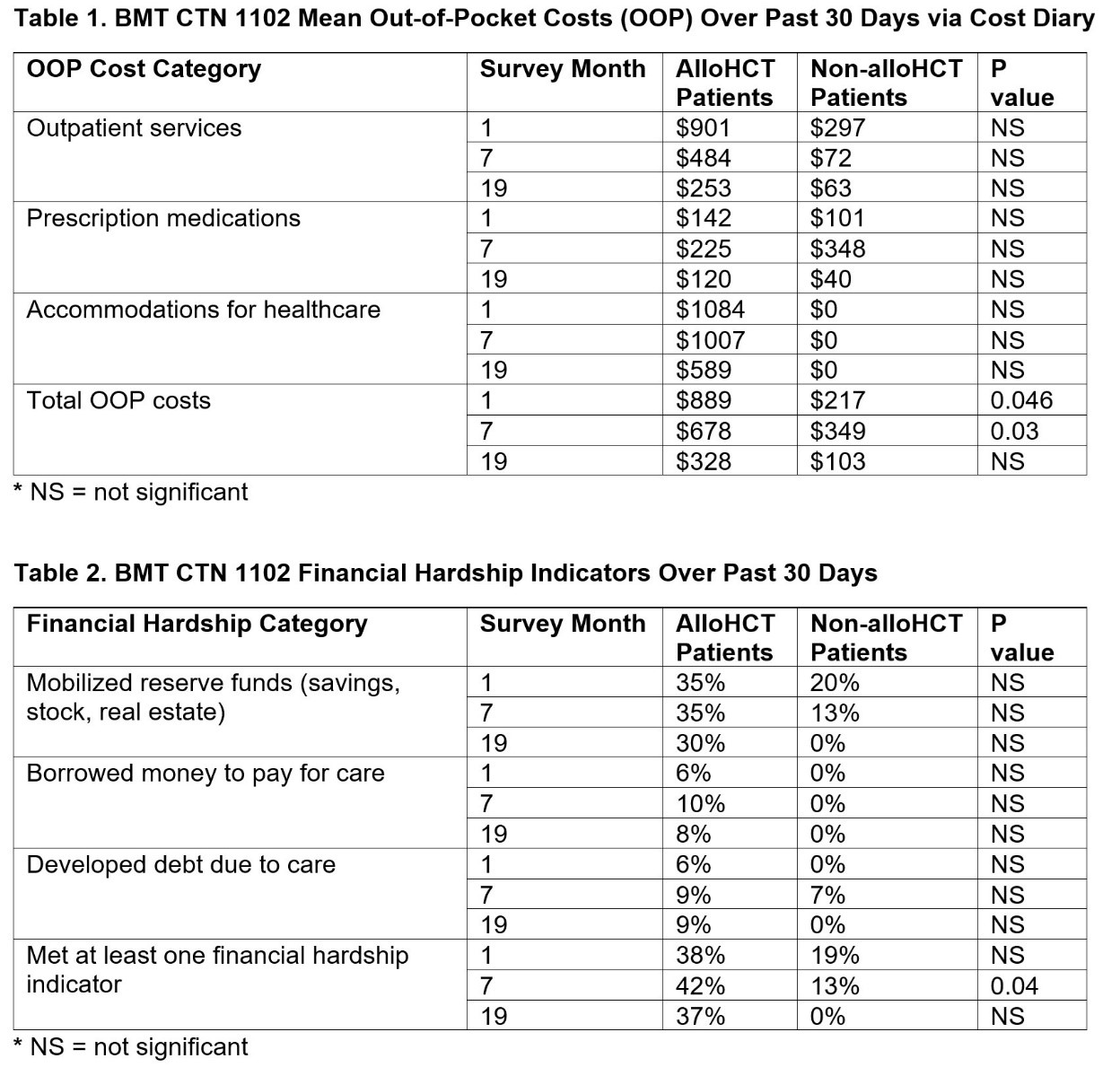
Su CT, et al., ASH abstract published in Blood
